AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
Back to Blog
Treatment of cataplexy8/9/2023  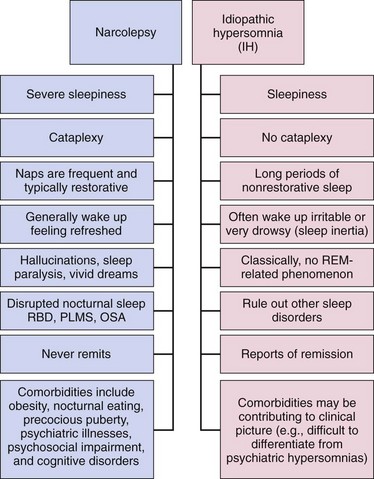 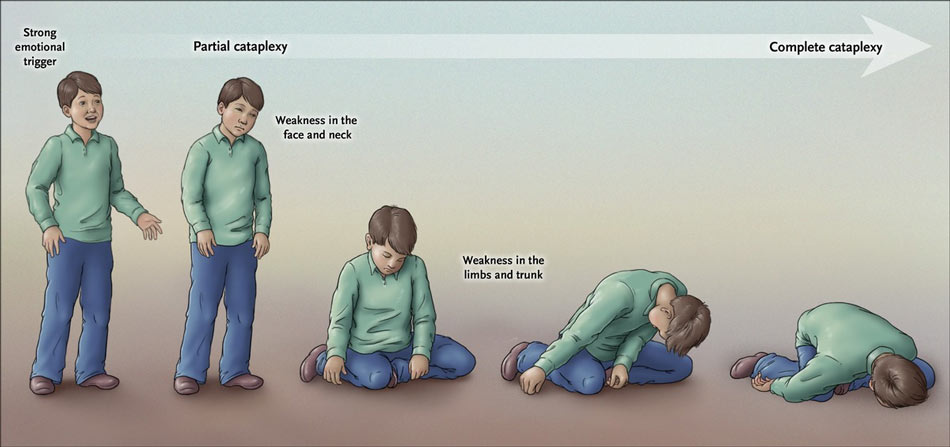
For this reason, it is still not possible to establish a concrete and extrapolable pattern. On one hand, it is important to note that when a patient develops symptoms, the hypocretinergic neurons may already present irreversible damage on the other hand, on average, there is a diagnostic delay of 10 years from the onset of symptoms. There is a clear variability in the evolution of the disease over time. This could be due either to their location in a restricted area where there is a small number of damaged antibodies, or because the activation of specific T cells is negligible. So far, no specific antibodies against ORX neurons have been detected. Genetically, approximately 98% of patients with NT1 carry the HLA class II allele DQB1*06:02 this allele is present in 50% of patients with NT2 and only 12–30% of the general population. Likewise, hypocretin deficiency reduces the excitatory signal of the neurons responsible for the synthesis of neurotransmitters that promote wakefulness, such as noradrenaline (NA), dopamine (DA), serotonin (5-HT) and histamine. The main symptoms of NT1 are related to hypocretin/orexin (ORX) deficiency, due to the selective destruction, likely autoimmune in origin, of ORX-producing hypothalamic neurons. 
If cataplexy develops over time or CSF orexin levels decrease to < 110 pg./ml, the diagnosis of NT2 must be change to NT1. Narcolepsy type 1 (NT1): EDS for > 3 months in association with either CSF orexin levels 3 months in the absence of cataplexy but with a mean sleep latency on the MSLT 110 pg./ml (or not measured). The current International Classification of Sleep Disorders (ICSD-3) defines two types of narcolepsy: Other sleep–wake symptoms are fatigue, sleep paralysis, hypnagogic and hypnopompic hallucinations, nightmares, lucid dreams, enacted dreams, disrupted night-time sleep, restless legs syndrome or parasomnias. Often is partial, rarely complete with falls. Narcolepsy presents with a variable combination of sleep–wake symtoms and motor, psychiatric, emotional, cognitive, metabolic and autonomic disturbances that reflect the hypothalamic origin of the disorder.Įxcessive daytime sleepiness (EDS), which can also manifest with sleep attacks, involuntary napping, automatic behaviours, difficulty sustaining attention and memory disturbances.Ĭataplexy, briefs episodes of bilateral loss of muscle tone triggered by sudden emotions in the presence of a normal state of consciousness. Narcolepsy is a chronic and disabling disease, which, according to the International Classification of Sleep Disorders (ICSD-3), considered to be hypersomnias of central origin. Other techniques such as hypothalamic stem cell transplantation, gene replacement therapy or immunotherapy are also being investigated. Future treatments include therapies based on the replacement of hypocretin or the administration of agonist receptors. 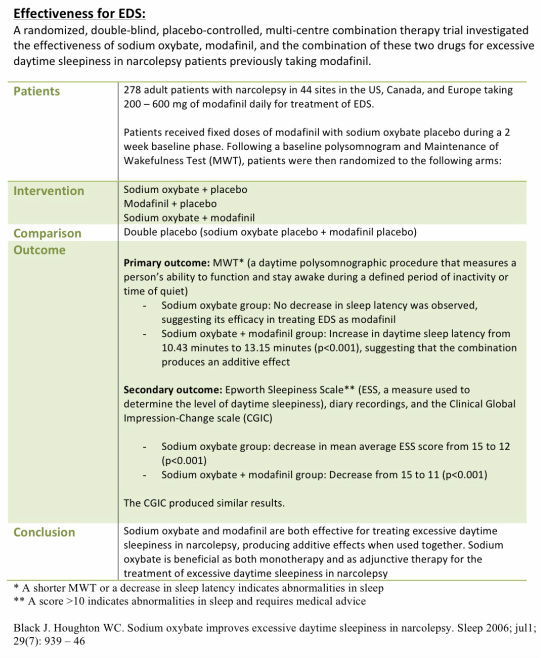
We intend to expose the different symptomatic treatments recommended by clinical guidelines and the clinical management from a practical point of view. On the other hand, pharmacological treatment must be individualised as there are great variations in severity, order of appearance symptoms and development of the disease. However, we have pharmacological treatments that effectively help control the main symptoms (excessive daytime sleepiness, cataplexy, fragmentation of nocturnal sleep, sleep paralysis and hypnagogic and hypnopompic hallucinations). Nowadays, treatment is focused on managing symptoms that impacts patient’s life, such as at workplace, social events or even at school, but not aimed cure the disease. Narcolepsy is a chronic, disabling sleep disorder with a significant diagnostic delay. 
0 Comments
Read More
Leave a Reply. |
 RSS Feed
RSS Feed
